Abstract
Introduction: To develop a preliminary, decision-making protocol capable of predicting sperm retrieval success in non-mosaic Klinefelter’s syndrome (KS) patients. Main outcome measure was to identify predictors of successful sperm retrieval and to build a decision-making protocol capable of predicting this success by assessing several variables including age, testicular volume, and preoperative hormonal responses. Methods: A retrospective cohort study included all men with non-mosaic KS who were treated with recombinant hCG and then underwent microdissection testicular sperm extraction (micro-TESE) between December 2019 and March 2023. Results: Thirty-eight patients who were treated medically with rec-hCG prior to their micro-TESE were included. Sperm was retrieved successfully from 28 (73.7%) patients. Initial testosterone differences between the groups were small and not significant, the mean pre-op (post-hormonal treatment) testosterone between the two groups was significant (p = 0.001). We then built a decision-making tree, in which testosterone change was the primary determining factor for successful sperm retrieval, testicular volume was a contributory secondary variable, and age was a tertiary consideration in cases of low testicular volume. Using this model, we observed the highest success rates (97%) in men with testosterone change of 9 nmol/L or more and testicular volume of 3 cc or more. on the other hand, men with no testosterone change with hormonal treatment, low testicular volume who were 25 years old or more had a success rate of only 63%. Conclusion: This study proposes a preliminary, decision-making protocol capable of predicting sperm retrieval success in non-mosaic KS patients. This model can be used as part of an individualized counseling approach. External validation is essential to corroborate our preliminary results.
Introduction
Klinefelter’s syndrome (KS) is the most frequent chromosomal abnormality in men, and 0.1–0.2% of males are affected [1]. About 90% of the cases are due to the 47,XXY karyotype, and the remaining 10% show a 46,XY/47,XXY mosaicism or higher grade X aneuploidies [2, 3].
Progressive testicular damage characterized by extensive fibrosis and hyalinization of the seminiferous tubules, which lead to impaired sperm production, is a major characteristic of KS. Approximately 90% of affected adult men suffer from nonobstructive azoospermia (NOA), and about 10% experience subfertility due to oligospermia [4]. These patients typically present with bilaterally symmetric, small, firm testes, and hypergonadotropic hypogonadism [5].
Men with non-mosaic KS may benefit from assisted reproductive technology due to the presence of residual foci with preserved spermatogenesis. With the availability of surgical sperm retrieval (SSR) combined with intracytoplasmic sperm injection (ICSI), half of the men diagnosed with non-mosaic KS can father their own genetic offspring [6‒8].
For KS patients, Leydig cells are generally considered dysfunctional and unable to produce adequate levels of testosterone, despite high levels of circulating luteinizing hormone (LH) [9]. Human chorionic gonadotropin (hCG) acts on the same receptor as LH and is considered more potent than LH on the cAMP signaling pathway [10]. Belli et al. [11] demonstrated that Leydig cells of KS men responded to hCG stimulation and that the first steps of steroidogenesis were fully functional, although testosterone production in these men was impaired.
Intratesticular testosterone (ITT) is required for several critical steps associated with spermatogenesis and spermiogenesis. These steps include the transition from type A to type B spermatogonia and, later, meiosis completion, adhesion of elongated spermatids to Sertoli cells, sperm release, and maintenance of the blood-testis barrier [12‒15]. In view of the pivotal role of testosterone in the regulation of spermatogenesis and spermiogenesis, elevation of ITT may contribute to the optimization of these processes. Hence, NOA patients who present with low circulating testosterone may benefit from hormonal optimization prior to their SSR [16, 17]. Although it has become a common practice to optimize production of endogenous testosterone before extraction of testicular sperm, the extent to which this contributes to enhancing sperm retrieval rates in KS patients remains unclear [17‒19].
Several clinical and biochemical parameters have been described as potential predictors of successful SSR in KS patients [18‒22]. Ramasamy et al. [23] reported that KS patients who required preoperative hormonal therapy and who responded to that treatment had a higher sperm retrieval rate than those who did not respond. Madgar et al. [21] also reported that a favorable response to hCG treatment was an important predictive factor of spermatogenesis in patients with non-mosaic Klinefelter syndrome. In their recent retrospective cohort study, Guo et al. [18] concluded that although therapy with hCG had no effect on SSR or ICSI outcomes in non-mosaic KS patients, preoperative testosterone levels, whether treated with hCG or not, predicted the chance of sperm retrieval with micro-TESE.
The understandable desire of non-mosaic KS patients who seek fertility treatments and who want to learn their chances of successful sperm retrieval necessitates thorough preoperative counseling. During these sessions, patients should be presented with substantial evidence to help them make an informed decision. The aim of this study was to develop a preliminary, decision-making protocol capable of predicting sperm retrieval success in non-mosaic KS patients by assessing their preoperative hormonal responses. This tool could provide valuable and relevant information for both patients and clinicians to use during individualized preoperative counseling.
Materials and Methods
The records of 38 consecutive non-mosaic KS patients who were treated with recombinant hCG and then underwent micro-TESE by a single surgeon (S.B.) between December 2019 and March 2023 were reviewed, retrospectively. Azoospermia was confirmed by two semen analyses based on WHO criteria [24] and two extended sperm searches, as described by Ron-El et al. [25].
The study was approved by the local institutional review board (0014-22-ASMC). Patients’ ages were recorded. Preoperative evaluation included a complete history, physical examination, body mass index, and routine scrotal ultrasound. Hormonal evaluation included serum testosterone, estradiol, LH, and follicle-stimulating hormone (FSH) hormonal analyses.
Blood samples were collected in serum tubes between 7:00 and 10:00 a.m. after 8–10 h of overnight fasting. The same laboratory and kits were used for all samples. Testosterone, estradiol, FSH, and LH levels were analyzed and quantified using a Siemens Advia Centaur XP. The laboratory reference ranges were 6.5–24 nmol/L for total testosterone, <223 pmol/L for estradiol, 1–9 IU/L for LH, and 1.4–18.1 IU/L for FSH. Patients with a testosterone level ≤14 nmol/L were included in the study [26]. All were treated with recombinant-hCG (rec-hCG-pen device) for ≥3 months prior to their surgery.
Treatment with rec-hCG was initiated at a dose of 2,500 iu twice weekly up to a maximum dose of 5,000 iu three times weekly. Hormonal treatment was continued until the time of micro-TESE.
Micro-TESE Procedure
Micro-TESE procedures were all performed by a single surgeon (S.B.). Following patient preparation and induction of general anesthesia, a skin cut was performed on the scrotal median raphe. Testicular envelopes of the larger testicle were opened, and a single testis was delivered through the incision. The tunica albuginea was incised widely in the equatorial plane, and microdissection was performed under a X20 magnification surgical operating microscope, as described originally by Schlegel and Li [27].
A systematic examination of testicular seminiferous tubules was then performed looking for dilated, opaque tubules. Once identified, tubules were removed using tissue micro-forceps and transferred to the embryology lab for further mechanical disintegration, followed by an initial sperm search. In cases where no thick or opaque tubules were found, systematic multiple micro biopsies were taken from the open testicle, which encompassed both upper and lower cut surfaces of superficial and deep areas.
Adequate hemostasis was achieved throughout the whole procedure using low-energy bipolar electrocautery. Once the testis was dissected sufficiently, the tunica albuginea was closed using running Vicryl 5/0 sutures. The tunica vaginalis was then closed with running Vicryl 4/0 sutures, and the testicle was placed back into its hemi-scrotum. If no sperm was found on the initial search, a similar procedure was performed on the contralateral testicle. The dartos layer was closed with running Vicryl 4/0 sutures, and skin edges were approximated with interrupted Vicryl Rapid 4/0. Cord block was performed for the operated side(s) with 20 mL 0.25% Bupivacaine solution.
Tissue Processing and Initial and Extended Sperm Search
Seminiferous tubules obtained during micro-TESE were first dissected mechanically under a stereomicroscope with the use of a bent 18-gauge needle. We used an inverted microscope at ×200 magnification for the initial search for spermatozoa. For an extended sperm search, dissected tubules were dissected further using a bent 18-gauge needle for another 20 min and then centrifuged at 1,000 g for 15 min. Most of the supernatant was removed, and about 0.5 mL was left above the pellet. The pellet was then resuspended back into the supernatant. Drops of 10–20 µL of the suspension were put in a FluoroDish (FD5040 – World Precision Instruments Inc.) and covered with light mineral oil (Oil for Embryo Culture – Irvine Scientific). The extended sperm search was performed with an inverted microscope (Olympus IX81) that was equipped with Nomarski optics, an Uplan Apo ×100 or ×40 objective lens, and a 0.55 NA condenser lens. Motile or immotile spermatozoa were collected with the use of an injection pipette and Eppendorf TransferMan Nk2 micromanipulator. The collected spermatozoa were placed in drops prepared in the same dish made of MHM-C medium (Multipurpose Handling Medium Complete – Irvine Scientific) supplemented with 30% human serum albumin (Irvine Scientific) for further injection into oocytes or cryopreservation.
Statistical Analysis
All analyses were performed using SPSS [IBM, ver. 29]. Descriptive statistics, distributions, and means were calculated for age, body mass index, LH, FSH, manual examination testicular volume, and initial and post-hormonal treatment testosterone (pre-op) levels and “testosterone change” (pre-op testosterone levels – initial testosterone levels). Paired t tests were performed between testosterone measures. Following these analyses, several combinations of the independent variables were tested and saved in a series of binary logistic regressions as potential predictors of sperm retrieval (i.e., IBM, SPSS c statistic). Of these, the combined prediction of “testosterone change,” age, and testicular volume that yielded the largest area under the curve (AUC) in a ROC analysis and that had the largest Cohen’s D effect were selected as the predictor of choice and used in all further analyses. To elucidate successful sperm retrieval by candidate typology, we then resubmitted the predicted probability into a “Decision Tree” analysis with age, testicular volume, and “testosterone change” recoded as ordinal variables to reveal the underlying differentiation of successful sperm retrieval.
Results
Thirty-eight patients with non-mosaic KS who were treated medically with rec-hCG prior to their micro-TESE were included in this study (Table 1). The mean age of subjects was 27.13 (range, 20–41). Sperm was retrieved successfully from 28 (73.7%) patients (SR+) and failed in 10 (26.3%) patients (SR−). Initial, pre-op, and change in testosterone levels were analyzed using sperm retrieval (Table 1).
Although initial testosterone differences between the SR+ and SR− groups were small and not significant, both the mean pre-op testosterone and the mean change in testosterone levels between the two groups were significantly different (p = 0.001 and p = 0.049, respectively). There was also a significant difference in testicular volume between the two groups (p = 0.032).
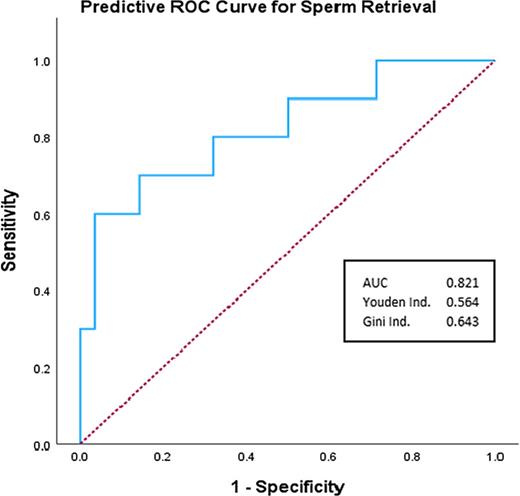
Several combinations of the independent variables were tested and saved in a series of binary logistic regressions as potential predictors of sperm retrieval. Of these, the combined prediction of “testosterone change,” age, and testicular volume yielded the largest AUC in a ROC analysis and the largest Cohen’s D effect, and this combination was selected as the predictor of choice used in all further analyses. AUC was calculated as 0.821 (CI: 0.658–0.984, p < 0.000, Fig. 1; Table 2); Youden Index was estimated at 0.564 at a sensitivity of 0.60 and a false-positive rate of 0.036. The calculation produced a Cohen’s D effect of 1.339.
To elucidate successful sperm retrieval by candidate typology, we then resubmitted the predicted probability into a “Decision Tree” analysis with age, testicular volume, and “testosterone change” recoded into ordinal variables by means of an optimal binning procedure. This revealed the progressive differentiation process of the sample by its essential constituents, which allowed us to propose an initial tentative ranking of patients with projected, sperm retrieval success.
Decision Tree Analysis
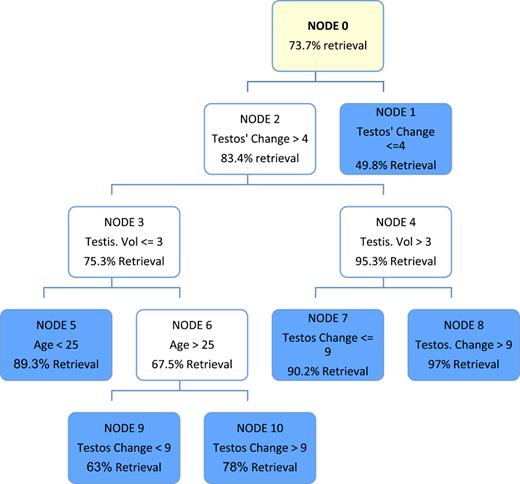
To produce a Tree Classification, the probability of sperm retrieval was entered into analysis as the dependent variable and age, testicular volume, and “testosterone change” were entered as independent variables after ordinal recoding. Because of the small sample size, no validation procedure was undertaken, and a Classification and Regression Trees (CRT)-based analysis was adopted to produce simple binary splits at every stage. The default level limit was specified, variable entry was not forced, and the analysis produced a 4-level tree with six terminal nodes, a risk estimate of 0.007, and a standard error of 0.002 (Fig. 2). For the complete detailed tree, see online supplementary Figure 1 (for all online suppl. material, see https://doi.org/10.1159/000550813).
Every terminal node of the tree defined a specific sample segment with a distinct sperm retrieval rate. Individuals with the lowest probability for success were patients whose “testosterone change” did not exceed 4 nmol [NODE 1], and individuals with the highest chances of success were patients with high “testosterone change” and high testicular volume [NODE 8]. “Testosterone change” was the primary determining factor for successful sperm retrieval, testicular volume was a contributory secondary variable, and age was a tertiary consideration in cases of low testicular volume.
Discussion
This study investigated the predictive value of preoperative hormonal response for successful sperm retrieval in non-mosaic Klinefelter patients treated with rec-hCG prior to their micro-TESE. We also propose a Decision Tree, classification analysis-based, prediction model for the successful sperm retrieval in this patient population. NOA due to progressive testicular damage represents a major challenge for KS patients. Most commonly, this is managed surgically. Basically, sperm retrieved from rare focal regions of spermatogenesis can then be used with ICSI. Micro-TESE, which is an effective and safe surgical technique, is currently considered a first-line approach for men with NOA who undergo sperm retrieval [28‒30].
Spermatogenesis is regulated by a complex network of endocrine and paracrine interactions that involve Sertoli, peritubular, Leydig, and germ cells. Testosterone plays a crucial role in this system, and it is essential for maintaining spermatogenesis [31]. In rodents, spermiogenesis relies heavily on ITT [32]. Additionally, a high level of ITT is crucial for the progression from type A to type B spermatogonia [14]. When testosterone activity is inadequate, spermatogenesis is blocked at the stages of meiosis and spermiogenesis, as demonstrated in studies using mice that lacked androgen receptors (AR knockout mice) [33, 34]. Although the ITT concentration necessary for optimal spermatogenesis in men with NOA is still unknown, ITT optimization may play an important role in the stimulation of spermatogenesis in men with NOA [35]. This is particularly relevant for KS patients, who typically present with lower serum testosterone levels than those seen in typical NOA cases. Some studies have demonstrated that KS patients who presented with hypogonadism benefited from hormonal stimulation prior to their SSR to maintain sufficient ITT levels, which improved the likelihood of effective sperm retrieval [16, 23, 35, 36].
A systematic review and meta-analysis conducted by Tharakan et al. [37] compared SSR rates in men with NOA, which excluded patients with hypogonadotropic hypogonadism, who received hormonal therapy compared with those who received a placebo or no treatment. Although a higher SSR was observed in subjects treated with hormones, a significant improvement was demonstrated only in normogonadotropic men. No such effect was seen in hypergonadotropic patients. Therefore, although the preoperative hormonal treatment among hypergonadotropic NOA patients remains controversial, many clinicians commonly adopt this practice, which also serves as our standard approach.
Our analysis consisted of 38 non-mosaic KS who were treated medically with rec-hCG prior to their micro-TESE. We observed an overall SRR of 73.7%. This finding was higher than those reported previously by others [8, 18, 22, 33, 34]. This may be attributed to the inclusion of a younger population in our study. Additional contributors may include our standardized preoperative rec-hCG stimulation protocol (administered for >3 months and continued until surgery), the performance of all micro-TESE procedures by a single experienced surgeon using a uniform technique, and a dedicated embryology workflow including extended sperm search. Nevertheless, given the modest sample size and single center retrospective design, these results should be interpreted cautiously and may not be fully generalizable. We share the view with others that performing sperm retrieval procedures at a younger age may result in favorable outcomes, considering the progressive seminiferous tubule hyalinization observed after puberty in KS patients. [35, 36]. Conversely, in their meta-analysis, Corona et al. [8] presented data that showed that successful sperm retrieval was independent of age. The authors supported their findings with published evidence, which suggested that impaired spermatogenesis in KS patients could also be caused by an intrinsic defect in the germ cells that was possibly linked to the (epi)genetics of the surplus X chromosome, rather than being a result of progressive hyalinization and fibrosis of the testicular environment [6, 35, 36].
Our analysis demonstrated that the combination of “testosterone change” that reflected hormonal response to hCG treatment, along with age and testicular volume, had good sensitivity and specificity for predicting successful sperm retrieval in KS patients who were treated medically prior to their micro-TESE (sensitivity: 60%, specificity: 96.4%, AUC: 0.821). These results are consistent with a recent report by Guo et al. [18], which found that among KS patients who received hCG treatment, patients with larger testicular volume who responded better to hCG were more likely to have a successful SR by micro-TESE.
We analyzed the combination of independent variables (i.e., age, testicular volume, and “testosterone change”) further by re-submitting the predicted probability into a “Decision Tree” analysis. Based on the presented Decision Tree analysis, patients with the lowest probability for successful SR were patients whose “testosterone change” did not exceed 4 nmol (predicted SR = 49.8%). Conversely, patients with the highest chances for successful SR were patients with high “testosterone change” and high testicular volume (predicted SR = 97%). In our study, “Testosterone change” emerged as the primary determining factor for successful sperm retrieval, with testicular volume as a contributory secondary variable and age as a tertiary consideration in cases of low testicular volume. We hypothesize that the higher preoperative “testosterone change” among successful KS NOA patients reflected more intact seminiferous tubules, which contained functionally normal Leydig cells with a preserved capacity to secrete testosterone. To the best of our knowledge, this is the first time a stepwise prediction protocol for successful sperm retrieval in KS patients has been proposed.
Proper counseling of KS patients who undergo micro-TESE is essential. Patients should be presented with solid evidence so proper decisions can be made and the psychological burden managed. Patients with a poor prognosis might decide to refrain from surgical treatment and consider other options, such as donor sperm or adoption. The suggested decision-making prediction model offers a straightforward, user-friendly tool that can assist clinicians during preoperative counseling sessions. It enables clinicians to distinguish more accurately among various phenotypes of KS patients, which provides each patient with a more customized prediction instead of the generic “50% chance” prediction often used.
We believe that KS patients with NOA may benefit from an individualized preoperative counseling approach. We suggest three supporting pillars for such counseling:
- 1.
The likelihood of a successful sperm retrieval (SR) based on current relevant literature.
- 2.
The likelihood of a successful SR based on the specific experience of the clinic/surgeons who will conduct the pre-operative hormonal treatment, using a local, up-to-date database.
- 3.
The likelihood of a successful SR based on the proposed decision-making, prediction protocol, which considers post-hCG treatment “testosterone change,” testicular volume, and age. This model can be used as a stand-alone predictive parameter or as an addition to predictors that were reported previously.
The limitations of this study were related primarily to its relatively small sample size. The proposed predictive model should be further validated to become more robust. Given the study’s retrospective design, it was not immune to selection bias. Additionally, the patient cohort featured homogeneous ethnicity, which suggested that our findings might not extend to KS patients across diverse ethnic backgrounds. Consequently, we advocate further studies that involve larger cohorts to ascertain the validity of this model. Despite these limitations, this study stands as the first to propose a straightforward, user-friendly prediction protocol for successful sperm retrieval in KS patients, and it marks an important contribution to the field.
In conclusion, this study proposes a preliminary, decision-making protocol capable of predicting sperm retrieval success in non-mosaic KS patients. The presented model considers the change in testosterone levels post-hCG treatment, along with testicular volume and age. This model can be used as part of an individualized counseling approach, either as a stand-alone predictive parameter or as an addition to predictors that were reported previously. External validation is essential to corroborate our preliminary results.
Acknowledgments
Thomas A. Gavin, Professor Emeritus, Cornell University, copy-edited the English in this paper.
Statement of Ethics
This study was approved by the Institutional Review Board of Assuta Ashdod University Hospital (Approval No: 0014-22-ASMC). All participants provided written informed consent. The research was conducted in accordance with the Declaration of Helsinki and adheres to the ethical standards outlined by the International Committee of Medical Journal Editors (ICMJE). All patients provided written informed consent to participate in this study and for their data to be used for research purposes. The study was conducted in accordance with the principles of the Declaration of Helsinki.
Conflict of Interest Statement
The authors have no conflicts of interest to declare. The authors declare no competing financial interests or personal relationships that could influence the work reported in this manuscript. All affiliations, funding sources, and institutional or corporate support relevant to this study have been transparently disclosed within the manuscript. This research complies with ethical standards and has been conducted with impartiality to advance knowledge in the urologic field.
Funding Sources
This study was not supported by any sponsor or funder.
Author Contributions
Conceptualization and writing – original draft: S.B. and S.D. Methodology: S.B, N.W., and S.D. Data curation: S.B., N.W., A.P., R.B., G.B., T.B.-M.B., O.B., and T.B. Formal analysis: S.B., N.W., and S.D. Writing – review and editing: all authors. Supervision: S.D. All authors reviewed and approved the final version of the manuscript.
Data Availability Statement
The data that support the findings of this study are not publicly available due to ethical and privacy restrictions but are available from the corresponding author upon reasonable request.