Abstract
Introduction: This meta-analysis compares the efficacy and safety of laser lithotripsy (LL) and pneumatic lithotripsy (PL) for upper tract urolithiasis. Methods: A systematic search of MEDLINE via PubMed, Embase, and the Cochrane Library identified trials comparing LL and PL. Primary outcomes included stone-free rate, operative time, and complications. A random-effects model was used, and heterogeneity was assessed using I2 statistics. Results: The systematic literature search identified 6,420 studies of which 43 fulfilled the inclusion criteria. The studies reported data from 7,377 patients. Random effect meta-analysis for stone free rate included data from 36 studies and yielded statistically significant higher stone free rates for LL with a pooled OR = 2.19 (95% confidence interval [CI] = 1.63–2.94, p < 0.001). Heterogeneity was substantial (I2 = 62%; p < 0.01). Random effect meta-analysis for operative time included data from 31 studies and yielded no statistically significant difference in operative time with a pooled MD = −1.09 min (95% CI = −4.39–2. 20, p = 0.5161). Heterogeneity was considerable (I2 = 98%; p < 0.01). Random effect meta-analysis for complications included data from 14 studies and yielded statistically significant fewer complications for LL with a pooled OR = 0.68 (95% CI = 0.48–0.96, p = 0.0276). Heterogeneity was limited (I2 = 27%; p = 0.17). Conclusions: LL might be superior to PL in upper tract urolithiasis therapy.
Plain Language Summary
Laser lithotripsy is more effective than pneumatic lithotripsy for the treatment of upper urinary tract urolithiasis (kidney and ureter) in adults as well as in children. Furthermore, laser lithotripsy is a safe procedure.
Introduction
The introduction and advances in intracorporeal lithotripter devices, especially laser and pneumatic devices have improved the stone-free rates after percutaneous nephrolithotomy (PCNL), retrograde intrarenal surgery (RIRS), as well as ureterorenoscopy (URS) for upper tract urolithiasis and at the same time decreased the risk of complications. These intracorporeal lithotripter devices work on different principles of stone fragmentation, e.g., the principle of pneumatic lithotripter consists of direct contact between the end of the rigid probe and the stone, the energy provided by a compressor being transmitted as compressed air to a metal projectile within the handpiece as pulses which is propelled to the end of the metallic probe resulting in stone fragmentation. In the early 90s laser lithotripsy (LL) systems have been introduced with the potential of being even more effective. Unfortunately, there is a lack of comprehensive evidence which system is more effective, not only in terms of stone-free rates, but also putting into account complications, quality of life (QoL), and cost effectiveness, especially in terms of a comprehensive meta-analysis [1‒5].
Consequently, we conducted a systematic review and meta-analysis addressing the following question: Are there any differences between LL versus pneumatic lithotripsy (PL) in upper tract urolithiasis concerning stone free rates, complications, and costs? Therefore, the primary aim of this study was to evaluate differences between LL and PL in primary outcomes such as stone-free rates and operation time and secondary outcomes such as complication rates. We also aimed to extract data for QoL and cost effectiveness.
Methods
Search Strategy
In May 2024, we performed a systematic literature search using MEDLINE via PubMed, Embase, and the Cochrane Library. The search algorithm broadly included the search term clusters urolithiasis, PCNL, URS and lithotripsy. The online supplementary material details the complete search algorithms (for all online suppl. material, see https://doi.org/10.1159/000550064). Reference lists of included articles, as well as review articles, were searched to identify additional records. No restrictions were made concerning language, study region, or publication type. Publication date was included after 1978, when the first pneumatic lithotripters were induced. This study was prospectively registered at PROSPERO (https://www.crd.york.ac.uk/prospero/; ID CRD 42024542375).
Study Inclusion and Exclusion Criteria
The predefined primary outcomes were visual stone-free rate, radiological stone-free rate, operating time, stone fragmentation time and length of hospital stay after stone lithotripsy (LL vs. PL) for upper urinary tract stones (ureter and kidney). We included randomized controlled trials (RCTs) as well as prospective clinical trial (non-RCTs) and retrospective cohort studies. Further exclusion criteria were not defined. The larger and more comprehensive publication was included if more than one publication evaluated the same patient cohort.
Data Extraction
An a priori defined standardized data extraction process was used for every included record. Extracted variables included author(s), year of publication, study country, population size, patient’s and stone characteristics, statistical methods, as well as absolute and relative data of effect (see primary and secondary aims). Study extraction was independently performed by two review authors. Inconsistencies were resolved by a third review author. The online platform covidence (https://www.covidence.org/; Veritas Health Innovation Ltd, Melbourne, Australia) was used for the screening and data extraction process.
Study Quality Assessment
Two reviewers independently assessed the risk of bias with the ROBINS-I-tool or the Cochrane Risk of Bias tool RoB2 as appropriate [6]. The ROBINS-I tool includes seven domains of bias: risk of bias due to confounding, bias in the selection of participants into the study, bias in classification of interventions, bias due to deviations from intended interventions, bias due to missing data, bias in the measurement of outcomes, and bias in the selection of the reported results for one outcome measurement. The domains are combined to an overall risk of bias. The RoB2 tool summarizes five risk of bias domains: bias arising from randomization process, bias due to deviations from the intended intervention, bias due to missing outcome data, bias in measurement of the outcome and bias in selection of the reported results. These domains are also combined to an overall risk of bias. Any disagreements were resolved by the involvement of a third review author.
Statistical Analysis
Comparison of the differences in predefined outcome parameters (primary and secondary) was performed using the inverse variance method weighting for pooling of continuous outcome data to account for clinical heterogeneity [7]. In all provided analyses, PL was considered the referent. Between studies, heterogeneity was assessed by the I2 statistic with the associated 95% confidence interval (CI), the chi-square p values of heterogeneity and visual inspection of forest plots. Heterogeneity was interpreted as limited – I2 = 0–40%, moderate – I2 = 41–60%, substantial – I2 = 61–80% and considerable I2 = 81–100%. Subgroup analyses were conducted to identify potential sources of heterogeneity. In addition, change of pooled hazard ratio over the years of publication was assessed. Publication bias was assessed by visual inspection of the funnel plot and by Egger's test. All statistical analyses were performed with R version 4.2.1 (https://www.r-project.org/) and RStudio (RStudio, Boston, MA, USA) and the R package meta. The alpha level indicating statistical significance was predefined as 0.05 for all analyses except the assessment of heterogeneity, which was considered at alpha = 0.1. All provided p values are 2-sided.
Results
Study Characteristics
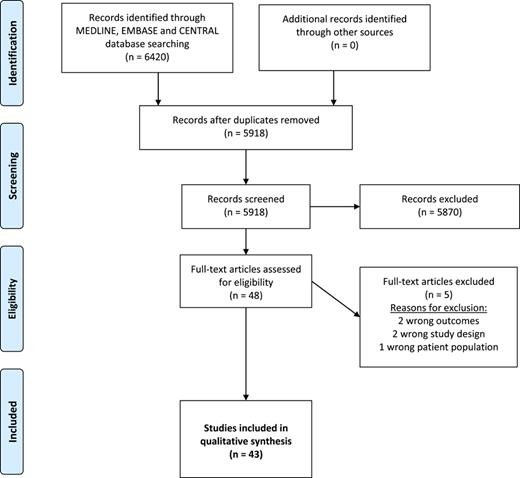
The systematic literature search identified 6,420 studies of which 43 fulfilled the inclusion criteria. Figure 1 presents the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) flowchart. The characteristics of the included studies are summarized in the SP [8‒50].
The studies were published between 2000 and 2024 and reported data 7,377 patients. All studies were published in English language. The majority of the studies were full-text articles, whereas only 3 studies were conference abstracts. The study size ranged from 36 to 880 patients.
A total of 26 studies were cohort studies, while 17 studies were RCTs. Almost half of the studies (n = 21) were designed as prospective studies. The majority of the studies were monocentric, while only three derived data from a multicentric setting. The study regions were mostly Asia (n = 24), followed by Europe (n = 10) and Middle East (n = 8).
The outcomes evaluated were stone-free rate (39 studies), late stone-free rate (10 studies), operative time (34 studies), length of hospital stay (24 studies), double J (DJ) stenting (5 studies), complications (19 studies), stone migration (5 studies), blood loss (3 studies), fragmentation time (4 studies) and costs (3 studies). Pooling was possible for the outcomes stone-free rate (36 studies), late stone-free rate (8 studies), operative time (31 studies), length of hospital stay (18 studies), DJ stenting (5 studies), complications (14 studies), stone migration (5 studies), and fragmentation time (4 studies).
Pooled Analysis for Stone-Free Rate
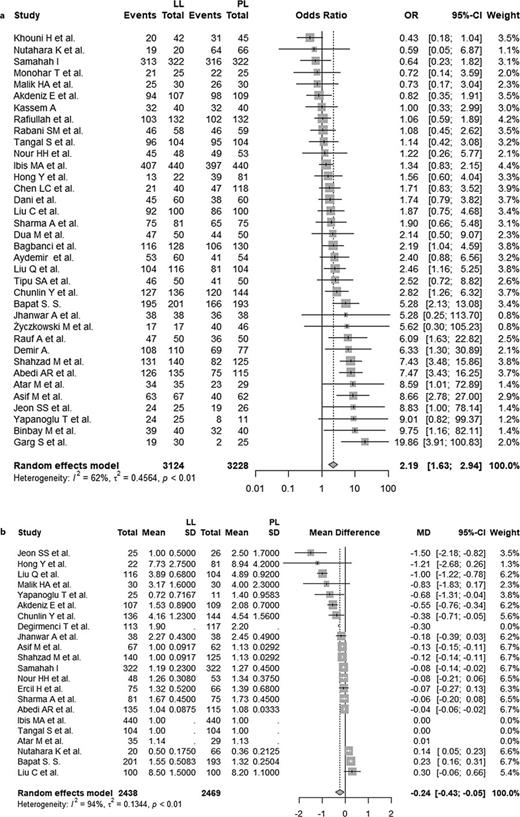
Random effect meta-analysis for stone-free rate included data from 36 studies and yielded statistically significant higher stone-free rates for LL with a pooled OR = 2.19 (95% CI = 1.63–2.94, p < 0.001). Heterogeneity was substantial (I2 = 62%; p < 0.01). This analysis is illustrated in Figure 2. Visual inspection of the funnel plot and Egger's test yielded no evidence of publication bias (Egger's test p = 0.1026), see online supplementary Figure A.
Pooled Analysis for Late Stone-Free Rate
Random effect meta-analysis for late stone free rate included data from 8 studies and yielded statistically significant higher stone free rates for LL with a pooled OR = 2.39 (95% CI = 1.51–3.80, p < 0.001). No relevant heterogeneity was found (I2 = 0%; p = 0.84). Visual inspection of the funnel yielded no evidence of publication bias. This analysis is illustrated in online supplementary Figure B.
Pooled Analysis for Operative Time
Random effect meta-analysis for operative time included data from 31 studies and yielded no statistically significant difference in operative time with a pooled MD = −1.09 min (95% CI = −4.39–2. 20, p = 0.5161). Heterogeneity was considerable (I2 = 98%; p < 0.01). Visual inspection of the funnel plot and Egger's test yielded no evidence of publication bias (Egger's test p = 0.4477). This analysis is illustrated in online supplementary Figure C.
Pooled Analysis for Length of Hospital Stay
Random effect meta-analysis for length of hospital stay rate included data from 18 studies and yielded a statistically significant shorter hospital stay for LL with a pooled MD = −0.24 days (95% CI = −4.39–2. 20, p = 0.5161). Heterogeneity was considerable (I2 = 98%; p < 0.01). This analysis is illustrated in Figure 2. Even though visual inspection of the funnel plot suggested publication bias with the true estimate lying even closer to a MD of 0, Egger's test yielded no evidence of publication bias (Egger's test p = 0.4542), see online supplementary Figure D.
Pooled Analysis for DJ Stenting
Random effect meta-analysis for DJ stenting included data from 5 studies and yielded statistically significant fewer stenting for LL with a pooled OR = 0.19 (95% CI = 0.07–0.48, p < 0.001). Heterogeneity was considerable (I2 = 85%; p < 0.01). Visual inspection of the funnel yielded no evidence of publication bias. This analysis is illustrated in online supplementary Figure E.
Pooled Analysis for Complications
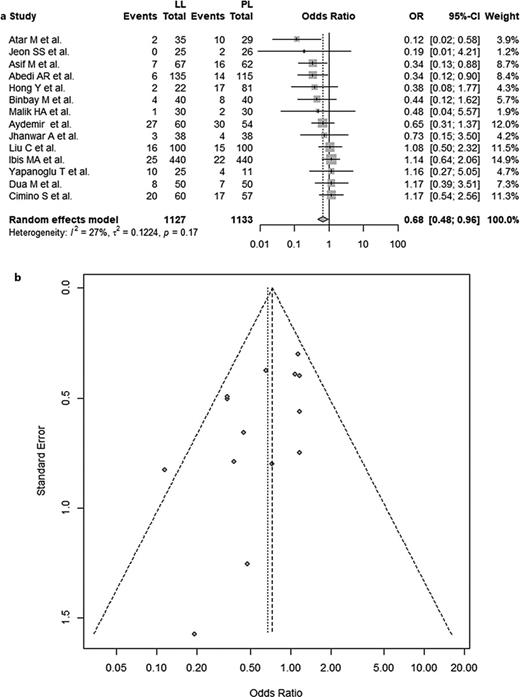
Random effect meta-analysis for complications included data from 14 studies and yielded statistically significant fewer complications for LL with a pooled OR = 0.68 (95% CI = 0.48–0.96, p = 0.0276). Heterogeneity was limited (I2 = 27%; p = 0.17). Visual inspection of the funnel plot suggested publication bias with the true estimate lying closer to an OR of 1 and Egger’s test yielded evident publication bias (Egger’s test intercept = 0.4454, t = −2.25, p = 0.0440). This analysis is illustrated in Figure 3.
Pooled Analysis for Stone Migration
Random effect meta-analysis for stone migration included data from 5 studies and yielded no statistically significant difference in stone migration rates with a pooled OR = 0.93 (95% CI = 0.19–4.58, p = 0.9276). Heterogeneity was considerable (I2 = 91%; p < 0.01). Visual inspection of the funnel plot did not suggest any publication bias. This analysis is illustrated in online supplementary Figure F.
Pooled Analysis for Fragmentation Time
Random effect meta-analysis for fragmentation time included data from 4 studies and yielded no statistically significant difference in fragmentation time with a pooled MD = −0.26 min (95% CI = −3.40–3.93, p = 0.8875). Heterogeneity was considerable (I2 = 95%; p < 0.01). Visual inspection of the funnel plot did not suggest any publication bias. This analysis is illustrated in online supplementary Figure G.
Subgroup Analyses
A detailed subgroup analysis including stone-free rates, operative time, length of hospital stay, and complications is given in the SP. Subgroup analyses for operative time revealed that some of the heterogeneity was driven by the laterality of the stones. Among the 3 pooled studies including only unilateral stones (vs. uni- and bilateral or bilateral only), statistically significant shorter operative time was evident for PL with a pooled MD = 5.31 (95% CI = 4.00–26.62). No Heterogeneity was evident (I2 = 0%; p = 0.84). The results of the subgroups analysis are depicted in the online supplementary appendix Figure I.
Furthermore, and due to clinical relevance, we performed analyses comparing the urinary tract access. Of the studies including PCNL only versus RIRS only: Of the 43 included studies, 37 studies (86%) reported results from RIRS only, whereas a total of six studies reported results from PCNL only. None of the studies mixed both access types. The subgroup analyses for stone free rate showed that some of the heterogeneity was driven by urinary tract access. Among the six pooled studies with PCNL, no statistically significant difference between LL and PL was evident anymore (OR = 1.40, 95% CI: 1.01–1.95) with an I2 = 0%; p = 0.88. Additionally, subgroup analyses for complications revealed that some of the heterogeneity was driven by urinary tract access. Among the four pooled studies with PCNL, no statistically significant difference between LL and PL was evident anymore (OR = 1.00, 95% CI: 0.64–1.55) with an I2 = 0%; p = 0.55.
Sensitivity Analyses
Cumulative meta-analysis for stone-free rate and late stone-free rate showed statistically significant effect from 2009 onwards, for stone migration since 2018, for length of hospital stay since 2022, for complications and for fragmentation time statistical significance was present from the beginning. The results of the sensitivity analysis can be found in online supplementary Figure L.
Non-Pooled Outcome Parameters (Expenses)
Hospitalization expenses in the study of Chunlin et al. [14]: PL is cheaper with a mean of CNY 8.24 thousand compared to LL with a mean of CNY 9.25 thousand (chi-square p = 0.014). Cost of surgery in the study of Demir et al. [17]: PL is cheaper with a mean of USD 2.16 (SD 66.13) compared to LL with a mean of USD 311.7 (SD 51.97), p = 0.001. Costs to attain stone-free status in the study of Nour et al. [36]: PL is cheaper with a mean of EGP 3404.11 versus LL with a mean of EGP 7,286.17, p < 0.001.
Detailed Information about Complications
More specific information about complications was available from several studies. Nutahara et al. [50] found statistically significant less days of postoperative gross hematuria in LL (mean 2.5 ± 1.8 vs. 4.3 ± 2.0 days, p < 0.01). Bapat et al. [48] found no statistically significant difference in urosepsis rates comparing PL and LL. Binbay et al. [12] found no difference in ureteral strictures. Kassem et al. [30] found no statistically significant difference in intraoperative perforation.
Further Study Aims
None of the studies reported QoL data or results from postoperative pain assessment.
Quality Assessment
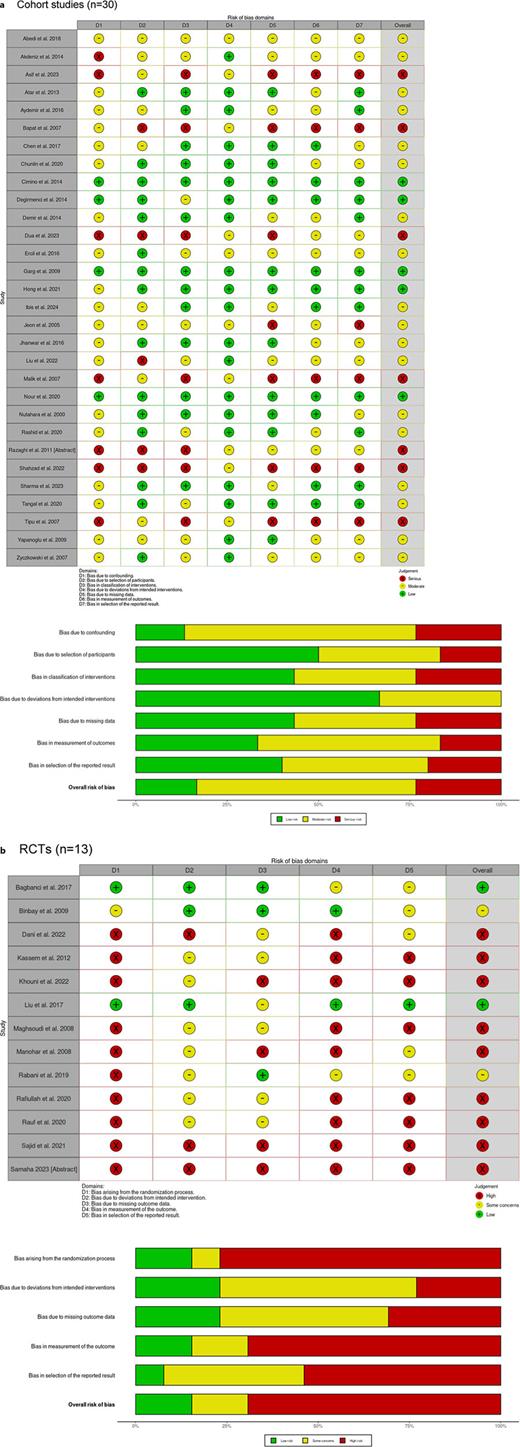
The overall risk of bias was moderate to high with reasons for limited quality being mainly due to retrospective study design of some studies and reporting bias. Figure 4 shows the detailed risk of bias assessment of the included studies.
Discussion
We conducted a systematic review and meta-analysis to assess differences in various outcomes, such as stone-free rate, operation time, and complications, between LL and PL. This topic is of great scientific interest as both techniques are used to treat urolithiasis of the upper urinary tract, and it remains unclear whether one intervention is superior to the other. However, the current European Association of Urology (EAU) guideline gives a strong recommendation to use holmium: yttrium-aluminium-garnet or thulium fiber laser LL for (flexible) URS or RIRS, but there is no explicit recommendation for PL, semirigid procedures or PCNL. Additionally, and to the best of our knowledge, this is first systematic review and meta-analysis addressing the question in upper tract stones and including adult patients as well as children.
The meta-analysis and the assessment of pooled data yielded several important findings: LL is superior to PL with respect to stone free rate and late stone free rate, complication rate, and fewer DJ stenting for LL. Yet, subgroup analyses for complication rates revealed no statistically significant difference for RCTs, studies with stones only in the kidney and studies with low risk of bias. However, the low numbers of pooled studies (twice 3 studies and once 5 studies) might have left the analyses underpowered. No difference in operative time except for unilateral stones where operative time was shorter for PL, length of hospital stay except for studies with bilateral stones only and RCTs and studies from the Middle East with a statistically significant shorter hospital stay for LL, stone migration, and fragmentation time. Nevertheless, our results are difficult to compare because, at least to our knowledge, there is no meta-analysis available addressing this question. Additionally, there were no significant differences in fragmentation time or stone migration rates. These nuanced findings support the idea that both devices may be suitable depending on the clinical scenario.
Our comprehensive subgroup analyses revealed some changes in effect size or statistically significance but the analyses for operative time remained the only case in which PL turned out to be superior to LL. In cases of missing statistical significance, the small size of some subgroups might have left the analyses underpowered what claims for further research on this topic to generate more evidence.
Unfortunately, no useful subgroup analyses were possible for publication language (all studies were published in English), abstract versus full publication (only three abstracts), uni- versus multicentricity (only three multicenter studies), type of laser used (only two studies with other than Holmium lasers), or adults versus children. Too few information was available for subgroup analyses by stone characteristics, previous therapies, risk of stone recurrence, and different types of PL used, e.g., PL together with a suction device.
However, the limitations of the analyzed data were that there was no pooling possible for cost effectiveness and there were no data available on pain assessment as wells as QoL data. Furthermore, the included studies did not report long-term outcomes, e.g., ureteral stricture rates, or recurrences of stones. Still, it would be of interest to also have information on the stone composition for choosing the best lithotripter device. Additionally, we reported that some of the heterogeneity was driven by the urinary tract access, so further research should focus on RIRS or PCNL alone when comparing lithotripter devices. Lastly, there was a great heterogeneity in the devices and their instrument settings.
On the basis of our findings, clinical implications are that LL seems to be more effective than PL with fewer complication rates, but subgroup analysis revealed that PL might be superior in operating time in complex bilateral stone disease. Additionally, there are hints from three studies that PL is more cost-effective than LL [14, 17, 36]. Consequently, further research is needed here addressing the question if PL might be the better and cheaper choice for complex and high stone burden in upper tract stones. Against the background of high economic pressure in the health care systems, this is of special interest. These further studies should also provide data on QoL, stone composition as well as long-term results.
We must assume that our study has also several limitations like the high risk in reporting bias and the heterogeneity of the included studies, so we attempted to mitigate this through detailed subgroup analyses and sensitivity testing, as documented in the SP. Our meta-analysis is the first to provide a head-to-head comparison of LL and PL in upper tract urolithiasis across both adult and pediatric and adult populations. It offers valuable insights and highlights areas requiring further investigation.
LL might be more effective and associated with fewer complications than PL in treating upper tract urolithiasis. However, PL may be more time-efficient in unilateral cases and more cost-effective in complex, bilateral, or high stone burden scenarios. These findings warrant further research to determine the optimal use of each modality, especially with respect to cost-efficiency, QoL, stone composition, and long-term outcomes.
Acknowledgments
The authors would like to thank Dr. Julia Lackner from UroEvidence from the German Society of Urology (DGU) for her guidance in the development of search strategies and validation of search strategies.
Statement of Ethics
Regarding this systematic review and meta-analysis, a statement of ethics is not applicable because this study is based exclusively on published literature.
Conflict of Interest Statement
All authors declare that they have no conflict of interest regarding this work.
Funding Sources
This review received no external funding.
Author Contributions
L.S. and A.U.: conception, data validation, analysis, and supervision. L.B., K.G.S., L.K., D.W., M.N.M., T.N., L.S., and A.U.: data extraction, critical review of the data, writing, and reviewing the manuscript.
Additional Information
Lujza Brunaiova, Karl G. Sommer, Laila Schneidewind, and Annemarie Uhlig contributed equally to this work.
Data Availability Statement
All data generated or analyzed during this systematic review and meta-analysis are included in this article and its supplementary material. Further inquiries can be directed to the corresponding author (L.S.).